Hesperian Health Guides
4. Sore throat, mouth sores, and thrush
HealthWiki > Helping Children Live with HIV > Chapter 12: Common health problems > Sore throat, mouth sores, and thrush
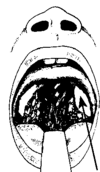
Sore throats are usually caused by a virus that leads to a common cold. The child’s throat may look red and may hurt when he swallows. The tonsils (which look like 2 lumps on each side of the back of the throat) may become large and painful, be covered in spots, or drain pus. Also, a thrush infection in the mouth can spread down the throat, making it feel sore (see Thrush).
Contents
Treatment for sore throat
- Give plenty of fruit juices, teas, and other fluids.
- Teach an older child how to gargle with warm salt water.
- Give paracetamol for pain.
For most sore throats, antibiotics will do no good and should not be used. But one kind of sore throat in children, strep throat, is dangerous, especially for children with HIV, and it is best to treat with antibiotics quickly.
Signs of strep throat
- Swelling, pus, and little white patches on the back of the throat
- Swollen or tender lymph nodes in the neck, below the ears
- Fever
- No cough or runny nose
Treatment for strep throat
If a child has the first 3 of these signs, but no cough or runny nose, the infection is likely to be strep throat. Treat with either penicillin OR amoxicillin.
GIVE
| Penicillin (Penicillin V or VK): Give 6 to 12 mg for each kg, 4 times a day, for 10 days. Or dose by age: |
| Under 1 year old: give 62 mg, 4 times a day, for 10 days. |
| 1 to 5 years old: give 125 mg, 4 times a day, for 10 days. |
| 6 to 12 years old: give 125 to 250 mg, 4 times a day, for 10 days. |
| Over 12 years old: give 250 to 500 mg, 4 times a day, for 10 days. |
OR GIVE
| Amoxicillin: Give 22 to 25 mg for each kg, 2 times a day, for 10 days. Or dose by age: |
| Under 3 months old: give 125 mg, 2 times a day, for 10 days. |
| 3 months to 3 years old: give 250 mg, 2 times a day, for 10 days. |
| 4 to 7 years old: give 375 mg, 2 times a day, for 10 days. |
Mouth sores and thrush
Children with HIV often get mouth sores. They can be painful and make it hard to eat. Be sure to check your child’s mouth for sores or discolored patches, especially if the child complains of mouth pain or is uncomfortable eating or drinking.
Treatment for mouth sores
- Treat for pain. Give parametacol for pain. Giving the child pain medicine 30 minutes before eating can help him eat more.
- Use lidocaine to control pain by spraying it directly in a child’s mouth or rubbing it on gently with a clean cloth.
- Use a clean cloth and salty water to gently clean the sores. Older children can swish salt water or baking soda and water in their mouths and spit it out.
- Dab the mouth sore with Milk of Magnesia or cover it with a paste made of baking soda and water.
- Wash your hands before and after cleaning your child’s mouth.
- Offer soft foods and healthy drinks. Children need healthy food when they are sick if they are to get well. Feed them soft or mashed foods, such as bananas, eggs, soup, and porridge.
- Avoid citrus (oranges or lemons), pineapple, and spicy foods, which might irritate the sores.
- Feed cool and cold foods more than hot foods. This will hurt sores less.
- Encourage children to drink more.
- Keep breastfeeding, but clean nipples with gentian violet (see next paragraph).
- Paint gentian violet on sores with a clean cloth 3 times each day for angry red mouth sores. If your child’s mouth seems dried out from this treatment, add water to make the gentian violet half-strength. If you are breastfeeding, use gentian violet to clean your nipples 3 times a day as well.
- For white patches, see thrush.
Thrush
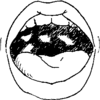
Thrush is a yeast or fungus infection in the mouth that can be very uncomfortable and painful. White patches inside the mouth are the most obvious sign. Thrush is very common in people with HIV who are not taking ART, including children.
Nursing mothers may feel pain or tingling in their breasts after nursing a baby with thrush. Looking in the baby’s mouth, you will see white or yellow patches surrounded by red skin. You can wipe the patches away but the skin around them remains red and sore. Sometimes the whole tongue is covered in white. Mouth pain makes babies with thrush very fussy. Older children complain about soreness in their mouth and do not want to eat, drink, or swallow.
Thrush can spread from the mouth into the throat, making it hard to swallow or breathe, and causing a burning feeling in the chest, especially after eating. Sometimes a child may vomit thick, white, mucus-like stuff. Treat thrush quickly to relieve pain, keep it from spreading, and help the child be able to eat.
Treatment for thrush
- Give paracetamol for pain.
- Make sure everyone in the household washes their hands carefully before and after helping treat a child. Thrush spreads easily.
- Dip a cloth in lightly salted water or vinegar, and gently wipe off the white patches. Do not press too hard — the skin around the white patches will be very sore.
- Gentian violet can also treat thrush sores. Use 0.5% gentian violet on white patches 3 times a day until 2 days after the thrush disappears.
GIVE
| Nystatin liquid, after meals: Give ½ ml of nystatin in each cheek, for 1 ml total, 4 times each day for 10 days. If thrush lasts longer than 10 days, continue treating until 2 days after thrush is gone. |
If the nystatin does not work, try fluconazole.
| Fluconazole: Give 3 mg for each kg the child weighs, one time a day, until it heals. Or dose by age: |
| Under 1 year old: give 25 mg (½ of a 50 mg tablet), one time a day, until it heals. |
| 1 to 3 years old: give 36 mg (¾ of a 50 mg tablet), one time a day, until it heals. |
| 4 to 7 years old: give 50 mg, one time a day, until it heals. |
| Note: Whether you use the weight-based or age-based dose, give a double dose the first day, then give the regular dose. |
When to get medical help for thrushIf thrush has spread to the throat and the child cannot swallow or has difficulty breathing, take her to a hospital or clinic as soon as possible. Other medicines will be needed. |
Mouth ulcers and gum infections:

Mouth ulcers are open sores that can appear anywhere in the mouth, especially on the inside of the lips. Usually the skin around the sores is much redder than the skin that is not broken. They can be painful and make talking and eating difficult. Healing can be very slow for children with HIV.
With gum infections, the skin around the teeth (the gums) becomes painful, red, and puffy, and may ooze yellow pus. Ulcers may develop between the teeth, and the child’s breath may smell very bad.
For both problems, keep the area clean with a cloth or cotton swab dipped in 1% povidone iodine, gentian violet, or 3% hydrogen peroxide mixed with clean water. Also give an antibiotic to children with swelling or pus in the mouth.
GIVE
| Amoxicillin: Give 44 to 50 mg for each kg, 2 times a day, for 5 days. Or dose by age: |
| Under 1 year: give 250 mg (one 250 mg tablet) ground up in a little breast milk, 2 times a day, for 5 days. |
| 1 to 3 years old: give 500 mg amoxicillin, 2 times a day, for 5 days. |
| 4 to 7 years old: give 750 mg amoxicillin, 2 times a day, for 5 days. |
OR GIVE
| Erythromycin: Give 10 mg for each kg, 4 times a day, for 3 days. Or dose by age: |
| Under 1 year: give 100 mg, 4 times a day, for 3 days. |
| 1 to 3 years old: give 150 mg, 4 times a day, for 3 days. |
| 4 to 7 years old: give 200 mg, 4 times a day, for 3 days. |
Take the child to see a health worker as quickly as possible if these problems do not improve, or keep the child from eating.
Red mouth sores and viral infections
Red sores in the mouth are common for children with HIV. They usually are caused by a virus, such as herpes. ART improves the immune system and helps to avoid viral sores. Treat all sores to help children be more comfortable and healthy while they heal.


