Hesperian Health Guides
How to prevent common illnesses
HealthWiki > Helping Children Live with HIV > Chapter 10: How to keep children healthy > How to prevent common illnesses
Contents
Give ART medicines every day
In order for HIV medicines to work, they must be taken every day, usually at the same time each day. Missing just 3 pills in a month can cause the child’s medicine to work much less well to fight HIV.
Giving your children their medication at the right times each day is very important for their health. As they get older, they can be more responsible for taking their medicine. See Chapter 11 for more about children and ART.
Help small babies stay warm
Babies born to mothers with HIV are often born too early and weigh too little (under 2.5 kg). Small or early babies get cold easily, which can be dangerous. They need help to stay warm.
Do not bathe any newborn baby in the first 24 hours after birth, and avoid bathing a small or weak baby often. When washing or bathing a baby, do it in a very warm room with warm water, and dry the baby well right away. Quickly wrap the baby, cover her head, and hold her close to warm her.
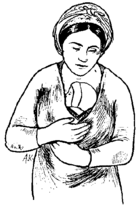
The best source of heat for a small or weak baby is the mother or caregiver. Wrap a small or weak baby next to your skin as much as possible, day and night. Sleep with the baby close. Check the baby regularly to see if her hands and feet are warm. If they are cold, wrap the baby close, skin-to-skin, to warm her.
When no skin-to-skin contact is possible, keep the baby clothed or covered as much as you can. Dress the baby with extra clothing, loosely wrap her in a soft dry cloth, and cover her with a blanket. Keep babies diapered (in nappies) and cover their heads and feet. Change any wet clothing quickly.
Give cotrimoxazole to prevent illness
Cotrimoxazole, also called Bactrim or Septrin among other brand names, is a very low-cost antibiotic that prevents pneumonia, malaria, diarrhea, and other infections in people with HIV, both children and adults. Cotrimoxazole can be a big help in keeping children with HIV healthy. However, any child with HIV also needs ART to stay healthy and should start taking ART as soon as possible. See Chapter 11.
Who should be given cotrimoxazole?
- Any baby under age 2 who has a positive HIV antibody test, or whose mother has HIV. (These both mean the baby might have HIV.)
- Any child 2 years or older with a positive HIV test.
- Any untested child who might have HIV, based on other illnesses he has.
You can give a baby cotrimoxazole starting as soon as 4 to 6 weeks after birth. Keep giving the medicine until you are sure the baby is not HIV positive, and cannot still become HIV positive through breastfeeding. To be sure a breastfeeding baby does not have HIV, you must test him 6 weeks after he stops breastfeeding. See Chapter 8 to read about how to know if a child has HIV.
Children who are HIV positive should keep taking cotrimoxazole until at least age 5. To give cotrimoxazole to babies and children who do or may have HIV, find the right dose in this chart and give it to the child once each day:
| Cotrimoxazole: A single-strength adult tablet of 480 mg contains 80 mg of trimethoprim and 400 mg of sulfamethoxazole | |||
| Child’s age | Using suspension (liquid) | Using suspension (liquid) | |
| 6 weeks to 6 months | 2.5 ml | ¼ tablet mix with breast milk or other milk | |
| 6 months to 5 years | 5 ml | Half tablet | |
| 6 years to 14 years | 10 ml | One tablet | |
| Older than 14 years | 2 tablets | ||
Prevent malaria
Malaria is an infection of the blood spread by mosquitoes. It is a serious problem for anyone, and is most dangerous for pregnant women and children.
When children with HIV get malaria, they become more ill than other children and may quickly develop other serious illnesses. See how to recognize and treat malaria in a child.
To prevent malaria

- Sleep under a bed net that, if possible, has been treated with insecticide. Caregivers and children should all sleep under bed nets. A healthy mother helps the whole family. And children learn by watching what adults do.
- Replace treated bed nets according to their instructions. They last different amounts of time.
- Check nets often for holes and repair them.
- Cover windows and doors with screens or cloths.
- If you have a fan, use it at night while sleeping or sitting around the house.
- Cover your skin when you go outdoors after the sun goes down.
- Treat anyone with malaria quickly. Signs may include fever, chills, headache, vomiting, and diarrhea. If you suspect malaria, go to a clinic to treat it as quickly as possible with the right medicines.
- Spray insecticides inside where mosquitoes rest — on walls, in corners, on the undersides of tables, and in closets. Do not spray insecticides on people, animals, or near water sources.
 |
| Tightly cover water containers. |
Community projects to prevent malaria
- Cover or drain standing water, which is where mosquitos breed. Get rid of old tires, cover empty barrels, and create drainage channels for water.
- Plant trees to give homes to birds that eat mosquitoes.
- Breed fish that eat mosquito eggs in ponds and lakes, such as guppies, gambusia, koi, or tilapia.
- Organize community clean-up efforts to keep mosquitos from breeding, getting in the house, and biting.
Prevent tuberculosis (TB)
Tuberculosis, or TB, is a dangerous disease that spreads easily, usually to the lungs, often causing a lasting cough. TB can also spread to other parts of the body, which happens more often in people with HIV than in people without HIV. TB can spread very easily between an adult who has it and a child living in the same house.
When someone has TB and HIV infection together, illness develops much faster than it does when he has only TB or only HIV. TB is the most common cause of death for people with HIV.
Children can get TB at any age, but it is most common in children between ages 1 and 4 years. The signs of TB can be difficult to see in children. If someone in a household has TB, any children in that household should be tested for TB, especially if they have HIV.
Signs in adults include a long-lasting cough (more than 3 weeks). Other signs are fever, sweating at night, and weight loss. In children, the only signs of TB may be steady weight loss or not growing well.
See information about TB and how to treat it.
To prevent TB in children:
- Give children lots of nutritious food. Children who are well fed do not get sick as easily from TB.
- Treat pregnant women, other caregivers, and any household members who have TB or HIV. Make sure people take the full treatment for TB.
- Use isoniazid, a medicine that can prevent TB. Any child under 5 years old who is living in a household where someone has TB should be given isoniazid. Children over 5 who have HIV should also take isoniazid. See more about this medicine.

- Keep fresh air flowing through your house.

Ack!
- People who are coughing or have untreated TB can pass it to children. After they have been on treatment for 2 to 4 weeks, it is safe for them to be around and sleep in the same room as children.
- Encourage everyone to cover their coughs. Cough into your elbow, not your hand, so you do not pass germs by hand later.
- If possible, stay away from crowded or enclosed areas. TB spreads most easily when people are crowded close together.
- Wash your hands often, especially after you cough.
- Do not spit indoors. Spit into a cup. If you spit on the ground outside, cover it with dirt.
Treat anyone who has signs of TB immediately. Treatment for TB takes several months, long after you feel better. But if you stop taking the medicine, the TB will come back, and it will be more difficult and costly to treat.
Prevent worms
Seeing worms in a child’s stool is common, and especially common in children with HIV. A child can also have worms without you ever seeing them. Worms can also sometimes cause severe rash and skin reactions. Children with worms may feel hungry more often.
Having worms is more serious when a child has HIV, because worms eat part of the child’s food and children with HIV already need to eat more. Worms may irritate the walls of the child’s stomach and intestines, increasing the chance of HIV infection if the child is still breastfeeding. Worm infections also overwork the immune system, which can make a child’s HIV infection worse.
 |
| Dirty hands sharing food can spread worms. |
Give children a regular dose of anti-worm medications every 6 months to prevent worm infections. The same medication will treat several types of common worm infections including roundworm, pinworm, and hookworm. Tapeworm needs a different medicine. See more on these medicines and doses.
Most worm infections are spread where it is difficult to use latrines, wash hands, purify water, or stay clean. These problems also cause food to become contaminated with worm eggs from an infected person’s feces.
Hookworm spreads through bare feet. Children should wear shoes to prevent contact with worms. Keep the toilet area clean, and make sure no food spills or scraps are left on the ground.
Immunizations
Immunizations (vaccines) protect children from serious diseases such as polio, measles, tetanus, and hepatitis. They must be given correctly and at the right times. It used to be thought that children with HIV should not get immunizations because their immune systems are weak. But exactly the opposite is true: immunizations are especially important for children with HIV, because the medicines help them fight or avoid infections. Boys and girls both need immunizations.
Some immunizations are “live” forms and may be less safe for a child with HIV. Make sure the health worker who gives an immunization knows your child is HIV positive or was born to an HIV-positive mother. Every country has guidelines for immunizing children with HIV.


